
Remnant cholesterol: new outcomes highlight its potential as a clinically useful cardiovascular risk factor
Introduction
Hypertriglyceridemia is a cardiovascular risk factor mainly thought to reflect increased plasma remnant lipoprotein particles, which contain a high proportion of cholesterol. This lipid readily accumulates during atherosclerosis and is the lipid usually measured as representative of blood remnant lipoproteins (1).
The concept of remnant lipoproteins (Figure 1) is indicative that lipoprotein particles originated during lipoprotein lipase (LPL)-mediated lipolysis of mature chylomicrons (generating smaller particles known as remnant chylomicrons) and very-low density lipoproteins (VLDL) generated remnant VLDL, also known as intermediate-density lipoproteins (IDL). IDL are at an intermediate stage, both in size and lipid content, between VLDL and low-density lipoproteins (LDL). The term “remnant cholesterol” has been also used as equivalent to VLDL cholesterol (VLDL-C), which is currently calculated or measured in the clinical laboratory (2,3).
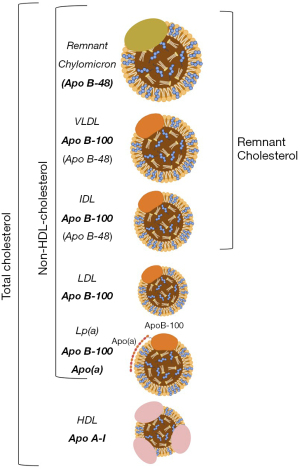
Remnant lipoproteins can be detected in fasting and, especially, in postprandial conditions (1-3). Classically, it has been thought that human lipoprotein particles originating from chylomicrons contain apolipoprotein (apo) B-48, whereas VLDL and IDL only contain the complete form of apoB (apoB-100). However, in recent years, it has been shown that the intestines secrete apoB48-containing particles not only as chylomicrons but also as VLDL, both in fasting and postprandial states. ApoB48-containing particles represent around 20–25% of VLDL and, especially in patients with hypertriglyceridemia, are slowly catabolized (4).
The hypothesis that increased remnant cholesterol (Figure 1) represents a risk factor for cardiovascular disease was first proposed by Donald B. Zilversmit in the 1970s (5). Even though type III hyperlipoproteinemia (a condition characterized by increased IDL concentration) was widely accepted as a highly proatherogenic disease long ago (6), the importance of remnant lipoprotein research was somewhat overshadowed by LDL and the consequent development of statins. However, in the last decade, and especially in the last few years, the hypothesis that remnant lipoprotein cholesterol is a risk factor for cardiovascular disease has been supported with novel results. In this editorial comment, we review only these recent findings as demonstrated by two papers published concomitantly in 2020 (2,3).
Clinical, epidemiological and mendelian randomization studies
As recently noted in a comprehensive review (7), levels of remnant cholesterol were associated with cardiovascular risk in older participants in the Atherosclerosis Risk in Communities Study and in a cohort from the Jackson Heart Study and the Framingham Offspring Cohort Study. Furthermore, it has been demonstrated that the cholesterol in triglyceride-rich lipoproteins is associated with peripheral artery disease risk (7). Moreover, different Mendelian randomization analyses have demonstrated that genetic variants that regulate remnant cholesterol plasma levels [either by codifying for apolipoproteins, such as APOC3; enzymes, such as LPL; or proteins that control LPL catabolism, such as angiopoietin protein-like 3 (ANGPLT3)] are causally associated with cardiovascular risk (7).
Primary prevention
Plasma cholesterol and triglycerides were measured using nuclear magnetic resonance (NMR) in VLDL, IDL, and LDL in about 25% of the 4-hour fasted samples of individuals that participated in the Copenhagen General Population Study (CGPS). The study therefore included 25,480 individuals with a mean age of 60 years who did not have experienced myocardial infarction or undergone lipid-lowering therapy at the beginning of the study. At the median follow-up of 11 years, 1,816 subjects were diagnosed with myocardial infarction (3). VLDL-C, which, as previously stated, was considered remnant cholesterol by the authors, explained 50% of the risk of myocardial infarction associated with apoB-containing lipoproteins, whereas IDL + LDL cholesterol explained 29%. The high association of LDL cholesterol (LDL-C) and IDL cholesterol (IDL-C) concentrations in this study explained its consideration as a unique variable. VLDL triglycerides, in contrast, were not associated with cardiovascular risk (3). Interestingly, the multivariable-adjusted hazard ratio (HR) of myocardial infarction obtained by increasing 1 mmol/L of VLDL-C (×38.61 to obtain cholesterol in mg/dL) was 1.71 and ranked first with respect to increasing 1 mmol/L of IDL + LDL-C (HR 1.32), smoking (yes vs. no, HR 1.31), and increasing 10 mmHg of systolic blood pressure (HR 1.11) (3). This does not necessarily have to be interpreted as remnant cholesterol being more important than LDL-C in inducing cardiovascular disease, as usually, LDL is the major cholesterol carrier in plasma.
In addition, in the context of the CGPS study, another investigation performed with 16,207 individuals directly explored whereas 4-hour fast measured remnant cholesterol was superior to calculated remnant cholesterol in predicting coronary heart disease (8). The calculated remnant cholesterol was, in fact, VLDL-C [remnant cholesterol = total cholesterol – high-density lipoprotein (HDL) cholesterol – LDL-C], with LDL-C calculated by the Martin-Hopkins method (9) rather than by the Friedewald equation. Remnant cholesterol was measured as the cholesterol in all triglyceride-rich lipoproteins using a recently developed, automated direct assay from Denka Seiken Co. Ltd. (8), which is traceable to the lipoproteins with density ≤1.019 g/mL and differs from a previous remnant assay by the same company (10). Directly measured remnant cholesterol identified 5% more of cases at risk than calculated remnant cholesterol (8). Importantly, in the CGPS, the inclusion of elevated remnant cholesterol levels improved heart disease risk prediction by 10% for myocardial infarction and by 5% for ischemic heart disease (11).
Step-wise higher remnant cholesterol concentrations were also associated with higher ischemic stroke risk in the CGPS and in the Copenhagen City Heart Study, with a multivariable adjusted HR of up to 1.99 for individuals with remnant cholesterol concentrations ≥1.5 mmol/L (~58 mg/dL) with respect to individuals with remnant cholesterol <0.5 mmol/L (~19 mg/dL). In this case, remnant cholesterol was calculated as the difference between total cholesterol minus LDL-C minus HDL-C (LDL-C was measured by direct methods when triglycerides >4 mmol/L; to obtain mg/dL, this value was multiplied by 88.5) (12).
Elevated remnant cholesterol in the CGPS and in the Copenhagen Heart City Study was associated with a five-fold increased risk of peripheral artery disease in the general population, which was more than twice that of myocardial infarction and ischemic stroke (13). Remnant cholesterol was calculated using LDL-C obtained by the Friedewald equation. Others formulas for calculating LDL-C, such as Martin-Hopkins or Sampson-NIH, provided very similar results (13).
In pooled data from 17,532 cardiovascular event-free individuals from the Atherosclerosis Risk in Communities study, the Multi-Ethnic Study of Atherosclerosis, and the Coronary Artery Risk Development in Young Adults, plasma remnant cholesterol was independently associated with atherothrombotic cardiovascular disease (14). Interestingly, the discordant high remnant cholesterol/low LDL-C group, but not the low remnant cholesterol/high LDL-C group, was associated with disease (14). In this study, the levels of remnant cholesterol were estimated as total cholesterol minus HDL cholesterol (HDL-C) minus calculated LDL-C using the Martin-Hopkins equation (14).
Secondary prevention or equivalent high cardiovascular risk
In the Spanish Predimed Trial, fasting remnant cholesterol (which was considered VLDL-C) calculated as triglycerides (mg/dL)/5 when the concentration of plasma triglycerides was <300 mg/dL, was also associated with major cardiovascular events, namely myocardial infarction, stroke, or cardiovascular death. The Predimed study included 6,901 men and women with a mean age of 67 years and a mean body mass index of 30 kg/m2 presenting with diabetes mellitus (48%) or three or more cardiovascular risk factors. The main goal of the study was to assess the effects of extra virgin olive oil and mixed nuts. There was a median follow-up of 4.8 years in which 263 events were detected (3.8%) (2). In a multivariable-adjusted analysis, an increase in 10 mg/dL (~0.25 mmol/L) of fasting remnant cholesterol was associated with an increased cardiovascular risk (HR of 1.21), similarly to non-HDL-C (HR 1.05) or triglycerides (HR 1.04), whereas no differences were observed for LDL-C and HDL-C (2). Fasting remnant cholesterol (or VLDL-C >30 mg/dL or 0.77 mmol/L) differentiated subjects at high risk of major cardiovascular events regardless of LDL-C being higher or lower than 100 mg/dL (2).
Direct measurement of remnant cholesterol using an automated assay (Denka Seiken Co. Ltd., Seiken) was performed in 4,355 patients from China with angiographically confirmed coronary artery disease during a median follow-up of 5.1 years. Adding this information resulted in better prediction of the 543 events that occurred during this period (10). In another study from the same country, 19.2% of the 94,869 Chinese patients hospitalized for acute coronary syndrome presented elevated remnant cholesterol (>1 mmol/L) (15).
A post hoc analysis of the Action to Control Cardiovascular Risk in Diabetes (ACCORD) trial, which included around 10,000 participants followed for a median of 8.8 years, assessed the associations between remnant cholesterol and cardiovascular outcomes in patients with type 2 diabetes. After adjusting for traditional cardiovascular risk factors, each unit of standard deviation (SD) increase in remnant cholesterol was associated with a 7% higher risk of major adverse cardiovascular events. In addition, remnant cholesterol ≥31 mg/dL identified individuals at a higher major adverse coronary event risk, regardless of LDL-C concentration (16).
In patients with type 2 diabetes, chronic kidney disease, and incident diabetic nephropathy, remnant cholesterol was associated with a higher risk of cardiovascular-related death (17). Similar results were also observed in long-term kidney transplant recipients (18).
Remnant cholesterol was independently associated with the risk of metabolic dysfunction-associated fatty liver disease and predicted all-cause, cardiovascular, and cancer-related mortalities in the NHANES III study (odds ratio of 1.71) (19). Remnant cholesterol concentration has also been independently linked to several cardiometabolic risk factors, even though it remains to be established whether this relationship is causal. For instance, remnant cholesterol has been shown to have a strong positive correlation with diabetes and with the risk of complications such as neuropathy and nephropathy (20,21), as well as with diabetes and fatty liver disease occurrence and severity (22).
Laboratory tests for clinical practice
The most frequently used method to establish the concentration of plasma remnant cholesterol (or VLDL-C) is calculating total cholesterol minus HDL-C and LDL-C. This follows the Friedewald equation, which is used in clinical assistance since the results resemble (in the absence of lipoprotein disorders) those obtained by measuring cholesterol in VLDL isolated by sequential ultracentrifugation (density ≤1.006 g/mL), a context in which IDL-C is usually included within LDL-C. Calculating remnant (or VLDL) cholesterol would involve the same imprecision as the measurement needed for calculation, namely triglycerides in the case of the Friedewald equation. Direct LDL-C determination or application of other formulas (Martin-Hopkins, Sampson-NIH) are also options to measure LDL-C and, afterwards, calculate remnant (or VLDL) cholesterol as total cholesterol – (LDL-C + HDL-C). In the latter case, remnant (VLDL) cholesterol calculation would be impacted by the imprecision of all the components used of the formula.
A second option is the use of a test from Denka Seiken Co. Ltd. (to our knowledge, not still commercially available), a direct automated method for measuring cholesterol from chylomicrons, VLDL, and IDL, which can be added up to obtain the remnant cholesterol. This method has been used in some of the studies reviewed in the present comment, but direct comparison with calculated remnant cholesterol only allowed for the identification of 5% more patients with increased concentration with respect to the calculation (8). A third option, used by some of the studies reviewed in this report, was NMR, a method that at this time remains unavailable to most clinical laboratories. Finally, and despite not being widely available (e.g., none of the studies reviewed here used it), measuring cholesterol in triglyceride-rich lipoproteins isolated by sequential ultracentrifugation (density ≤1.019 g/mL) may also be an option.
In Table 1, one can observe that there are differences between studies, both in the methodologies for measuring or calculating remnant (or VLDL) cholesterol and in the fasting period, which contrast with the quite consistent results showing, as explained, that remnant cholesterol concentration is associated with cardiometabolic risk. Thus, overall, remnant cholesterol information lent value to several studies compared to the more traditional parameters used in a clinical laboratory setting, including LDL-C, non-HDL-C, triglycerides, or apoB-100. It is, however, unclear yet whether remnant cholesterol is superior to other parameters that may provide (at least partly) similar information, such as apoC-III, LDL triglyceride, or ANGPTL3 concentrations (7,10,23,24). Certainly, the calculation of remnant cholesterol rather than experimental determination of the other biomarkers might provide an advantage through its simplicity and lack of cost, but some of these other biomarkers (i.e., apoC-III or ANGPTL3) are directly targeted by drugs in current development, which could favor their use in the future.
Table 1
| Author, country (studied population), reference | Context | Individuals/patients | Fasted plasma | Measurement method |
|---|---|---|---|---|
| Balling et al., Denmark (3) | Primary prevention, 11-year follow-up | 25,480 | 4-hour fast | NMR |
| Remnant cholesterol (VLDL-C) calculated as TG/2.2 (when TG <4 mmol/L), or calculated after direct LDL-C measurement (when TG >4 mmol/L) as Remnant cholesterol = TC – (LDL-C + HDL-C) | ||||
| Varbo et al., Denmark (8) | Primary prevention, 4-year follow-up | 16,207 | 4-hour fast | Not commercially available Denka Seiken method, RLP-C |
| Remnant cholesterol (VLDL-C) = TG/2.2 (when TG <4 mmol/L), or calculated (when TG >4 mmol/L) as Remnant cholesterol = TC – (LDL-C + HDL-C) with LDL-C estimated with the Martin-Hopkins formula | ||||
| Varbo et al., Denmark (12) | Primary prevention, 14-year follow-up | 102,964, reconfirmed in 9,548 more | 4-hour fast | Remnant cholesterol (VLDL-C) calculated as TG/2.2 (when TG <4 mmol/L, or calculated after direct LDL-C measurement (when TG >4 mmol/L) as Remnant cholesterol = TC – (LDL-C + HDL-C) |
| Doi et al., Denmark (11) | Primary prevention, 10-year follow-up | 41,928 | 4-hour fast | Remnant cholesterol (VLDL-C) calculated as TG/2.2 (when TG <4 mmol/L, or calculated after direct LDL-C measurement (when TG >4 mmol/L) as Remnant cholesterol = TC – (LDL-C + HDL-C) |
| LDL-C was also calculated by the Martin-Hopkins or the Sampson-NIH formula | ||||
| Wadström et al., Denmark (13) | Primary prevention | 106,397 | 4-hour fast | Remnant cholesterol (VLDL-C) as TG/2.2 (when TG <4 mmol/L), or calculated after LDL-C measurement (when TG >4 mmol/L) as Remnant cholesterol = TC – (LDL-C + HDL-C). LDL-C was also calculated by the Martin-Hopkins or the Sampson-NIH formula |
| Quispe et al., USA (14) | Primary prevention, 18.7-year follow-up | 17,532 | Overnight | Remnant cholesterol (VLDL-C) = non-HDL-C – Martin-Hopkins calculated LDL-C |
| Castañer et al., Spain (2) | High CVD risk, 4.8-year follow-up | 6,901 | Overnight | Remnant cholesterol (VLDL-C) as TG/2.2 (when TG <3.39 mmol/L) |
| Cao et al., China (10) | High CVD risk, 5.1-year follow-up | 4,355 | Overnight | Not commercially available Denka Seiken method, RLP-C |
| Fu et al., USA and Canada (16) | High CVD risk, 8.8-year follow-up | 10,196 | Overnight | Remnant (VLDL) cholesterol = non-HDL-C – LDL-C |
| Yu et al., China (17) | High CVD risk, 2-year follow-up | 2,282 | Overnight? | Remnant cholesterol (VLDL-C) as TG/2.2 |
| Jansson Sigfrids et al., Finland (21) | High CVD risk, up to 17-year follow-up | 5,150 | Light fasting | Remnant cholesterol (VLDL-C) = TC – (Sampson-NIH formula calculated LDL-C + HDL-C) |
| Hussain et al., USA (23) | High CVD risk, up to 6-year follow-up | 6,359 | Overnight | Not commercially available Denka Seiken method, RLP-C |
CVD, cardiovascular disease; HDL-C, high-density lipoprotein cholesterol; NIH, National Institutes of Health; NMR, nuclear magnetic resonance; LDL-C, low-density lipoprotein cholesterol; TC, total cholesterol; TG, triglycerides; RLP-C, remnant lipoprotein particle-cholesterol; VLDL-C, very-low-density lipoprotein cholesterol.
Conclusions and perspectives
Consistent results indicate that increased plasma remnant cholesterol is a risk factor for cardiovascular disease both in primary and secondary prevention and seems particularly indicative of peripheral artery disease risk. Mendelian randomization analysis suggests causality. There are indications that remnant cholesterol might improve patient risk classification. Large, randomized trials of triglyceride- and remnant cholesterol-lowering treatment are needed in order to know whether they can further reduce cardiovascular disease risk with respect to the current standard of care. The results of these interventional studies will likely determine whether and which specific laboratory tests (calculated or measured remnant cholesterol, apoC-III, or ANGPTL3), in addition to the standard lipid profile, are best suited for clinical practice and under which circumstances (overnight or 4-h) of fasting should be used. Further studies are also needed to understand the role of remnant lipoproteins in the development and prognosis of high cardiovascular risk in illnesses such as diabetes mellitus, obesity, and renal disease.
Acknowledgments
Funding: This work was supported by Instituto de Salud Carlos III and FEDER “Una manera de hacer Europa” PI21/00140 grant to MT and FB-V, and CIBERDEM, an initiative of the Instituto de Salud Carlos III.
Footnote
Provenance and Peer Review: This article was a standard submission to the journal. The article has undergone external peer review.
Peer Review File: Available at https://jlpm.amegroups.com/article/view/10.21037/jlpm-22-70/prf
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at https://jlpm.amegroups.com/article/view/10.21037/jlpm-22-70/coif). FBV serves as an unpaid editorial board member of Journal of Laboratory and Precision Medicine from September 2021 to August 2023. The other authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Ginsberg HN, Packard CJ, Chapman MJ, et al. Triglyceride-rich lipoproteins and their remnants: metabolic insights, role in atherosclerotic cardiovascular disease, and emerging therapeutic strategies-a consensus statement from the European Atherosclerosis Society. Eur Heart J 2021;42:4791-806. [Crossref] [PubMed]
- Castañer O, Pintó X, Subirana I, et al. Remnant Cholesterol, Not LDL Cholesterol, Is Associated With Incident Cardiovascular Disease. J Am Coll Cardiol 2020;76:2712-24. [Crossref] [PubMed]
- Balling M, Afzal S, Varbo A, et al. VLDL Cholesterol Accounts for One-Half of the Risk of Myocardial Infarction Associated With apoB-Containing Lipoproteins. J Am Coll Cardiol 2020;76:2725-35. [Crossref] [PubMed]
- Björnson E, Packard CJ, Adiels M, et al. Apolipoprotein B48 metabolism in chylomicrons and very low-density lipoproteins and its role in triglyceride transport in normo- and hypertriglyceridemic human subjects. J Intern Med 2020;288:422-38. [Crossref] [PubMed]
- Zilversmit DB. Role of triglyceride-rich lipoproteins in atherogenesis. Ann N Y Acad Sci 1976;275:138-44. [Crossref] [PubMed]
- Paquette M, Bernard S, Baass A. Dysbetalipoproteinemia Is Associated With Increased Risk of Coronary and Peripheral Vascular Disease. J Clin Endocrinol Metab 2022;108:184-90. [Crossref] [PubMed]
- Hoogeveen RC, Ballantyne CM. Residual Cardiovascular Risk at Low LDL: Remnants, Lipoprotein(a), and Inflammation. Clin Chem 2021;67:143-53. [Crossref] [PubMed]
- Varbo A, Nordestgaard BG. Directly measured vs. calculated remnant cholesterol identifies additional overlooked individuals in the general population at higher risk of myocardial infarction. Eur Heart J 2021;42:4833-43. [Crossref] [PubMed]
- Martin SS, Blaha MJ, Elshazly MB, et al. Comparison of a novel method vs the Friedewald equation for estimating low-density lipoprotein cholesterol levels from the standard lipid profile. JAMA 2013;310:2061-8. [Crossref] [PubMed]
- Cao YX, Zhang HW, Jin JL, et al. Prognostic utility of triglyceride-rich lipoprotein-related markers in patients with coronary artery disease. J Lipid Res 2020;61:1254-62. [Crossref] [PubMed]
- Doi T, Langsted A, Nordestgaard BG. Elevated Remnant Cholesterol Reclassifies Risk of Ischemic Heart Disease and Myocardial Infarction. J Am Coll Cardiol 2022;79:2383-97. [Crossref] [PubMed]
- Varbo A, Nordestgaard BG. Remnant cholesterol and risk of ischemic stroke in 112,512 individuals from the general population. Ann Neurol 2019;85:550-9. [Crossref] [PubMed]
- Wadström BN, Wulff AB, Pedersen KM, et al. Elevated remnant cholesterol increases the risk of peripheral artery disease, myocardial infarction, and ischaemic stroke: a cohort-based study. Eur Heart J 2022;43:3258-69. [Crossref] [PubMed]
- Quispe R, Martin SS, Michos ED, et al. Remnant cholesterol predicts cardiovascular disease beyond LDL and ApoB: a primary prevention study. Eur Heart J 2021;42:4324-32. [Crossref] [PubMed]
- Yang N, Wang M, Liu J, et al. The Level of Remnant Cholesterol and Implications for Lipid-Lowering Strategy in Hospitalized Patients with Acute Coronary Syndrome in China: Findings from the Improving Care for Cardiovascular Disease in China-Acute Coronary Syndrome Project. Metabolites 2022;12:898. [Crossref] [PubMed]
- Fu L, Tai S, Sun J, et al. Remnant Cholesterol and Its Visit-to-Visit Variability Predict Cardiovascular Outcomes in Patients With Type 2 Diabetes: Findings From the ACCORD Cohort. Diabetes Care 2022;45:2136-43. [Crossref] [PubMed]
- Yu D, Wang Z, Zhang X, et al. Remnant Cholesterol and Cardiovascular Mortality in Patients With Type 2 Diabetes and Incident Diabetic Nephropathy. J Clin Endocrinol Metab 2021;106:3546-54. [Crossref] [PubMed]
- Horace RW, Roberts M, Shireman TI, et al. Remnant cholesterol is prospectively associated with cardiovascular disease events and all-cause mortality in kidney transplant recipients: the FAVORIT study. Nephrol Dial Transplant 2022;37:382-9. [Crossref] [PubMed]
- Huang H, Guo Y, Liu Z, et al. Remnant Cholesterol Predicts Long-term Mortality of Patients With Metabolic Dysfunction-associated Fatty Liver Disease. J Clin Endocrinol Metab 2022;107:e3295-303. [Crossref] [PubMed]
- Hu X, Liu Q, Guo X, et al. The role of remnant cholesterol beyond low-density lipoprotein cholesterol in diabetes mellitus. Cardiovasc Diabetol 2022;21:117. [Crossref] [PubMed]
- Jansson Sigfrids F, Dahlström EH, Forsblom C, et al. Remnant cholesterol predicts progression of diabetic nephropathy and retinopathy in type 1 diabetes. J Intern Med 2021;290:632-45. [Crossref] [PubMed]
- Zhang S, Cheng S, He X, et al. Remnant Lipoprotein Cholesterol as a Factor Related to Adult Fatty Liver Disease. J Clin Endocrinol Metab 2022;107:e1598-609. [Crossref] [PubMed]
- Hussain A, Sun C, Selvin E, et al. Triglyceride-rich lipoproteins, apolipoprotein C-III, angiopoietin-like protein 3, and cardiovascular events in older adults: Atherosclerosis Risk in Communities (ARIC) study. Eur J Prev Cardiol 2022;29:e53-64. [Crossref] [PubMed]
- Kou M, Ding N, Ballew SH, et al. Conventional and Novel Lipid Measures and Risk of Peripheral Artery Disease. Arterioscler Thromb Vasc Biol 2021;41:1229-38. [Crossref] [PubMed]
Cite this article as: Ferrer R, Mansilla A, Tondo M, Blanco-Vaca F. Remnant cholesterol: new outcomes highlight its potential as a clinically useful cardiovascular risk factor. J Lab Precis Med 2023;8:11.


